Circulating cell-free DNA in liver transplantation: A pre- and post-transplant biomarker of graft dysfunction
Damiano Patrono1, Monica Sorbini2, Tullia Carradori2, Gabriele Togliatto2, Cristiana Caorsi2, Morteza Mansouri3, Luisa Delsedime4, Elena Vissio4, Antonio Amoroso3, Renato Romagnoli1, Silvia Deaglio2.
1General Surgery 2U - Liver Transplant Unit, AOU Città della Salute e della Scienza di Torino, Turin, Italy; 2Medical Genetics, AOU Città della Salute e della Scienza di Torino, Turin, Italy; 3Regional Transplant Coordination Centre, AOU Città della Salute e della Scienza di Torino, Turin, Italy; 4Pathology Unit, AOU Città della Salute e della Scienza di Torino, Turin, Italy
Background: Reliable biomarkers are needed to assess graft dysfunction after liver transplantation (LT) and facilitate graft monitoring. This study investigated cell-free DNA cfDNA) as a pre-and post-LT marker of graft dysfunction.
Methods: Donor-derived cfDNA (dd-cfDNA) levels were determined at fixed timepoints in 45 consecutive LT recipients (baseline, from day 0 to day 7, week 2-3-4, 3 and 6 months). 22 (49%) patients received a graft treated by hypothermic oxygenated machine perfusion (HOPE) and 3 (7%) by normothermic machine perfusion. Perfusate levels of cfDNA and mitochondrial cfDNA (mt-cfDNA) were available for 20 recipients of a HOPE-treated graft. cfDNA and mt-cfDNA were correlated to other parameters of graft function and clinical outcome.
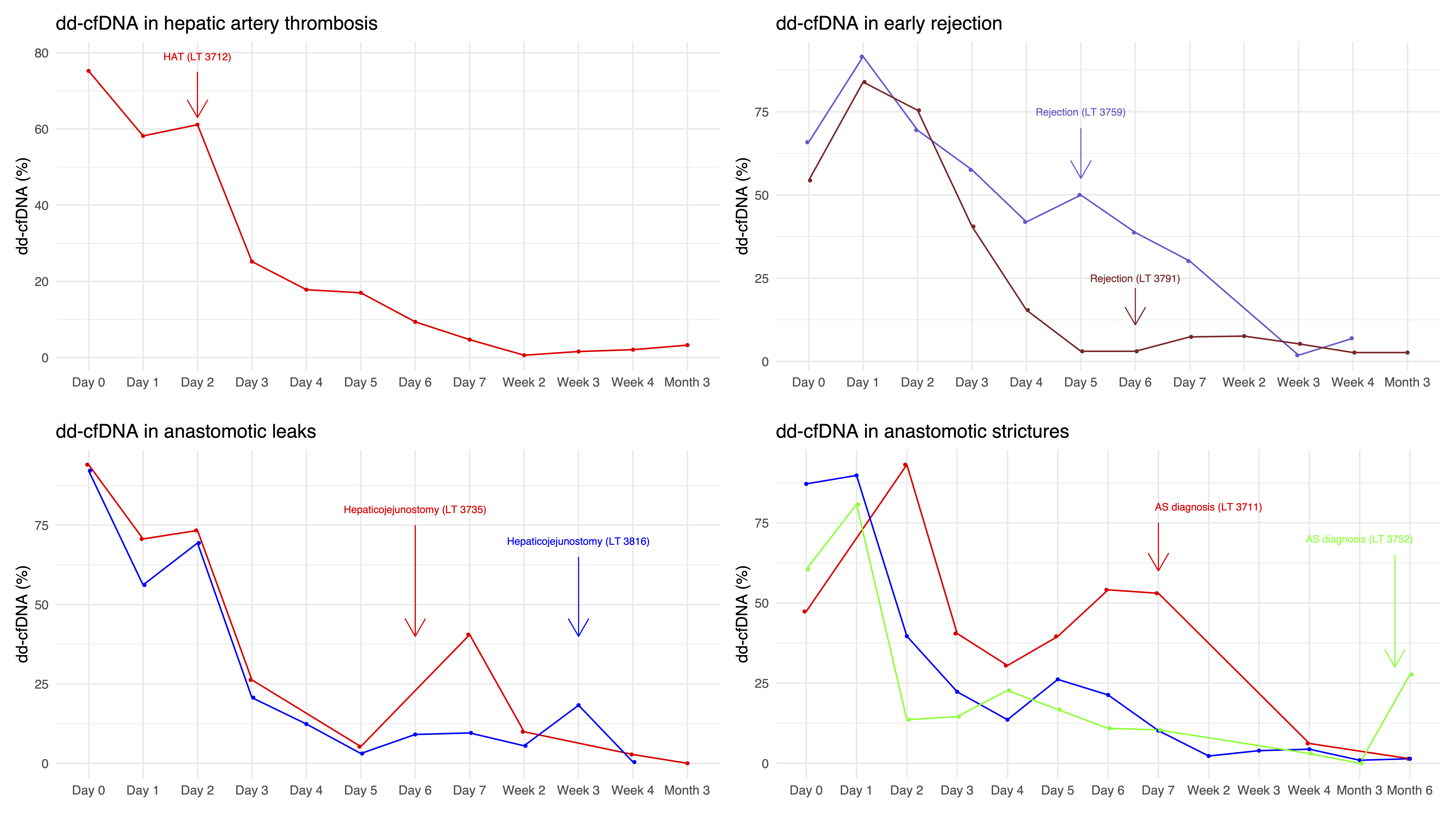
Results: 45 patients with median MELD-Na 15.4 were included. Hepatocellular carcinoma was the indication for LT in 21 (46.7%) patients. Trend of dd-cfDNA levels after LT was depicted. dd-cfDNA % peaked the day of LT and reduced over following days. Dd-cfDNA levels were not influenced by gender, cross-match, cold ischemia time, or preservation technique. Levels of dd-cfDNA correlated with the release of transaminases and the degree of histological reperfusion injury until postoperative day 5. Liver-related complications were associated with an increase of dd-cfDNA levels, possibly increasing diagnostic accuracy.
During HOPE, cfDNA and mt-cfDNA levels progressively decreased. Mt-cfDNA perfusate levels were positively correlated at all timepoints with perfusate flavin mononucleotide (FMN) levels and with parameters of graft injury and function post-LT (area under the curve of logAST; maximum INR).
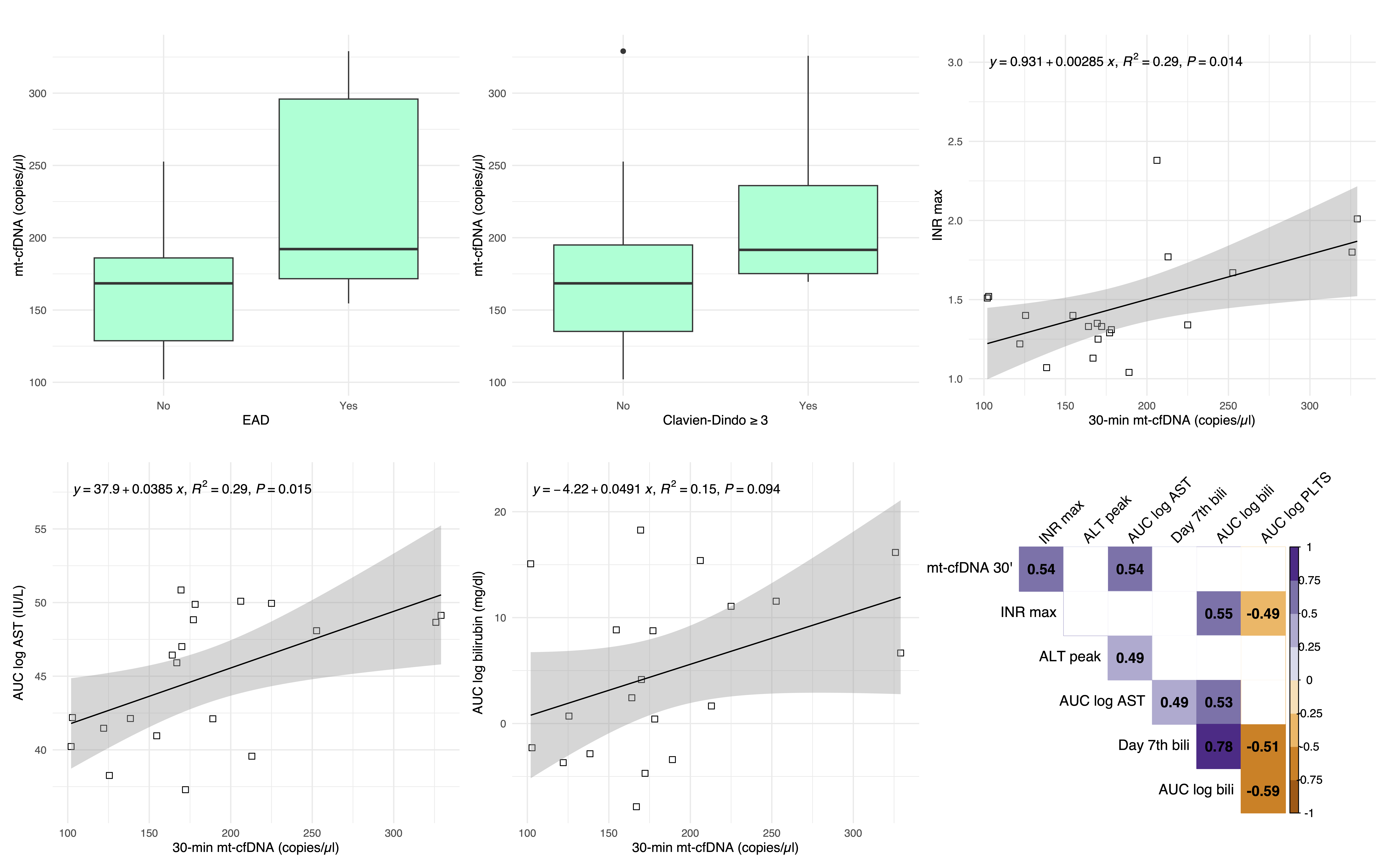
Conclusion: In LT, dd-cfDNA correlates with hepatocyte necrosis and represents an aspecific yet sensible marker of graft dysfunction. When HOPE is used, perfusate mt-cfDNA correlates with liver injury and function after LT and may represent a further tool of liver viability assessment.
[1] circulating cell-free DNA
[2] mitochondrial cell-free DNA
[3] ischemia-reperfusion injury
[4] graft monitoring
[5] machine perfusion
[6] hypothermic oxygenated machine perfusion
